Definition
Mastalgia is breast pain. There are two types of mastalgia or breast pain: cyclic and noncyclic. Cyclical breast pain is most often associated with menstrual periods. Noncyclical breast pain is not related to the menstrual cycle.
Causes
Mastalgia can be caused by:
- Hormonal changes associated with the menstrual cycle
- Pregnancy
- Trauma to the breast
- Mastitis
- Thrombophlebitis
- Stretching of breast ligaments
- Pressure from a bra
- Hidradenitis suppurativa
- Certain medications, such as hormone medications, antidepressants, or certain heart medications
Risk Factors
Factors that may increase your risk of having mastalgia may include:
- Having a history of breast surgery or breast injury
- Having large breasts
Symptoms
Symptoms of mastalgia may include pain in the breast area. Pain may be mild or severe. It may occur in both breasts or just one. It may be painful only in one spot or all over the breast.
When Should I See a Doctor?
Call your doctor right away if you have any signs of infection, such as redness, tenderness, fever, or chills.
Call your doctor if you notice any other changes in your breasts, such as:
- Change in the size or shape of your breast
- Discharge from your nipple
- New lumps or masses felt in the breast
- Other changes to the skin on your breasts, such as crusting, dimpling, or puckering
Call your doctor if your breast pain persists, interferes with your daily routine, or is in one specific area of your breast.
Diagnosis
Your doctor will ask about your symptoms and medical history. A physical exam will be done. The diagnosis is most often done with history of pain.
Your doctor may order further testing to look for any suspicious changes. These tests may include:
- Mammogram
- Ultrasound
- Breast biopsy
Treatment
Talk with your doctor about the best treatment plan for you. Treatment may be based on what is causing your breast pain. General treatment options include:
Medications
Topical nonsteroidal anti-inflammatory drugs (NSAIDS) may reduce the pain associated with mastalgia. Other medications may be prescribed to help reduce cyclical mastalgia.
If you are taking hormones, such as estrogen or progesterone, your doctor may make changes to your medications to reduce pain.
Other Treatments
Your doctor may suggest some changes depending on the cause of your breast pain. These might include:
- Wearing a properly fitting bra that has good support
- Avoiding caffeine
- Eating a low-fat diet
- Using a hot or cold compress
- Some health supplements you can buy in Kenya can help.
Prevention
There are no current guidelines to prevent mastalgia.

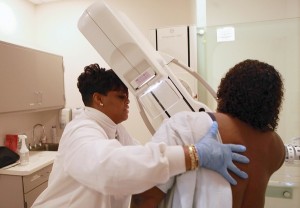 Patient teaching about Screening Mammogram involve: –
Patient teaching about Screening Mammogram involve: –

